Osimertinib is a highly effective treatment for non-small cell lung cancer. But it carries hidden risks.
A sudden cough might seem harmless at first. However, it could be an early sign of severe lung inflammation. Waiting too long to report these changes can be incredibly dangerous.
At Medicine for World, we believe knowledge is your best defense. This article breaks down exactly what symptoms to watch for and how to act fast to protect your respiratory health.
What is Osimertinib-Induced Pneumonitis?
Osimertinib targets specific EGFR mutations in lung cancer cells. It is a powerful tool against NSCLC. Sometimes, the drug mistakenly causes the immune system to attack healthy lung tissue.
This reaction causes drug-induced pneumonitis. Pneumonitis is simply inflammation of the lungs. It makes breathing difficult and reduces oxygen flow to your body.
How Common is Lung Inflammation with Tagrisso?
Patients often worry about experiencing this specific side effect. Severe, life-threatening cases are quite rare. FDA data and clinical trials show severe pulmonary toxicity happens in roughly 1% to 4% of patients.
Mild cases, however, are much more common. Up to 18% of patients develop asymptomatic pulmonary opacities. This means the inflammation shows up clearly on a scan but causes absolutely no physical problems.
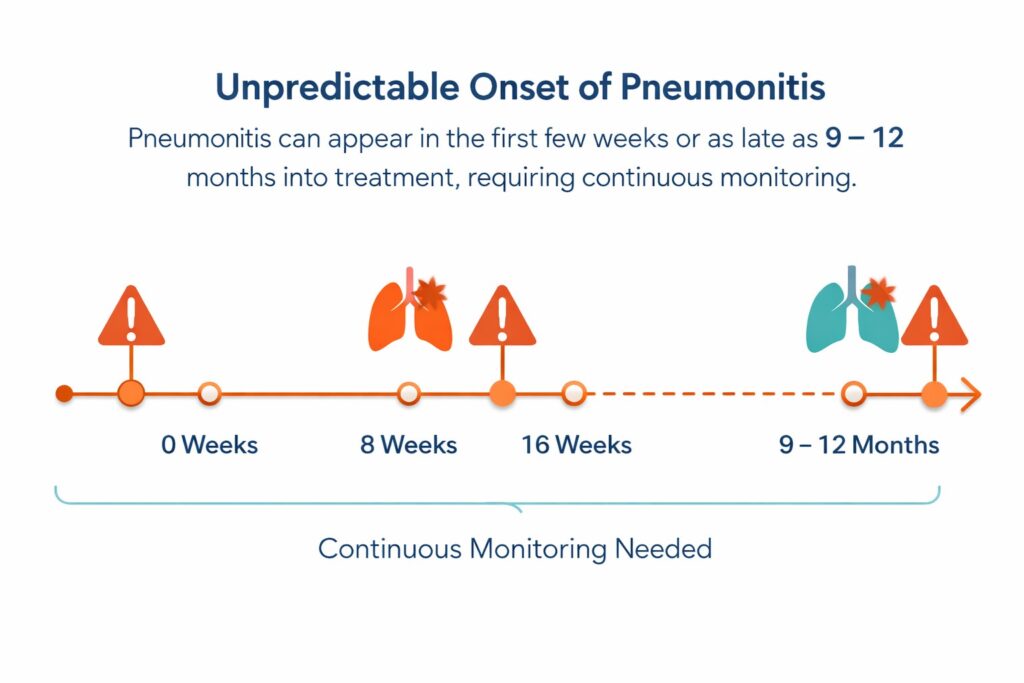
The Unpredictable Timeline and Early Warning Signs
You cannot predict when pneumonitis will strike. It can happen rapidly during your first week. It can also suddenly appear nine months into your treatment plan.
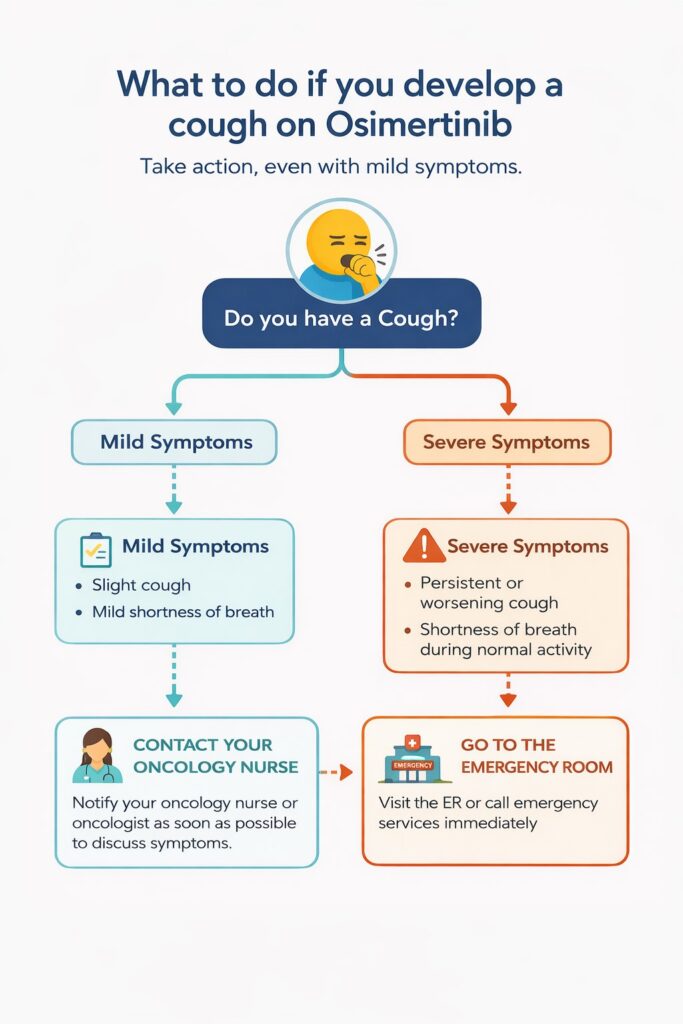
Because the timeline varies, you must stay vigilant. Watch closely for these core early warning signs:
- Persistent dry cough: A nagging cough that does not produce any mucus.
- Worsening shortness of breath: Feeling unusually winded while doing basic daily tasks.
- Dyspnea: Labored, difficult breathing even while you are resting.
- Unexplained fever: A sudden spike in your overall body temperature.
- Low blood oxygen levels: Often detected easily via a home pulse oximeter.
Who is at the Highest Risk for Pulmonary Toxicity?
Certain underlying factors greatly increase your chances of developing this condition. Your doctor will review your medical history closely before starting treatment.
Patients with a history of interstitial lung disease face the highest risk. A long history of heavy smoking also elevates your chances significantly.
Finally, prior immunotherapy treatments increase the danger. If you had treatments like durvalumab before starting osimertinib, your risk of inflammation goes up.
Diagnosis and Medical Management: What to Expect
If you report breathing issues, your oncology team will act quickly. They will immediately order a chest CT scan. This imaging helps doctors spot ground-glass opacities in your lungs.
The exact medical treatment depends on how severe your symptoms are.
| Severity Level | Patient Symptoms | Standard Medical Action |
| Mild (Grade 1) | None. Visible only on CT scan. | Continue osimertinib. Monitor lungs closely. |
| Moderate (Grade 2) | Cough or mild shortness of breath. | Hold treatment. Start oral corticosteroids. |
| Severe (Grade 3/4) | Severe breathing trouble. Low oxygen. | Permanent discontinuation. Hospital admission. |
The Road Ahead: Can You Restart Targeted Therapy?
Pausing your cancer treatment is terrifying for most patients. Many ask if they can ever safely restart the drug. Restarting the medication is formally called a rechallenge.
Doctors only try a rechallenge if your initial inflammation was very mild. Your lungs must heal completely on a scan first.
If you restart, your doctor will likely lower your dose. They may also prescribe preventative steroids to protect your lungs. Permanent discontinuation is always required for severe cases.
FAQ: Answering Your Top Questions
What are the symptoms of pneumonitis from osimertinib?
The most common symptoms include a persistent dry cough, worsening shortness of breath, unexplained fever, and low blood oxygen levels. Contact your doctor immediately if these occur.
These signs closely mimic regular chest infections like pneumonia. Never ignore them. Early detection is absolutely vital for your safety and recovery.
How common is lung inflammation with Tagrisso?
Severe lung inflammation from Tagrisso occurs in about 1% to 4% of patients. Mild, symptom-free inflammation visible only on scans affects up to 18% of patients.
Most patients tolerate the targeted therapy extremely well. However, the potential severity means routine chest imaging is always a required safety measure.
Who is at the highest risk for osimertinib lung toxicity?
Patients with preexisting interstitial lung disease, a history of smoking, or those who previously received immunotherapy face the highest risk of developing severe lung toxicity.
Your oncology team will thoroughly screen for these specific factors before prescribing the medication to minimize your overall respiratory risks.
How do doctors treat drug-induced pneumonitis?
Doctors first pause the targeted therapy. They then prescribe systemic corticosteroids like prednisone to reduce inflammation quickly. Severe cases may require hospital admission and supplemental oxygen therapy.
Fast medical action prevents permanent and dangerous lung damage. Always follow your doctor’s exact instructions regarding your steroid dosages and tapering schedules.
Can you restart osimertinib after pneumonitis?
Yes, but only in mild cases. This is called a rechallenge. Doctors typically prescribe a lower dose and add preventative steroids to stop inflammation from returning.
If you experienced severe, life-threatening lung inflammation, your doctor will permanently stop the medication and find safer alternative cancer treatments.