Bunions are a prevalent foot ailment, but they are still often misunderstood, and their impacts are considerable, including reduced mobility, discomfort, and lowered quality of life. In mild cases, changes in footwear or the use of orthotics can manage the symptoms, while progressive bunions may necessitate surgery for correction. Remarkably, minimally invasive bunion surgery has replaced the traditional methods for treating the condition, giving patients the benefits of its faster recovery and better cosmetic outcomes.
Potential patients not only look for the best surgical options but also the best surgeons, so they often turn to specialists who perform minimally invasive foot surgery in London. These modern techniques are increasingly being used to treat bunions and associated toe deformities, providing accurate results with minimal tissue disruption.
What is a Bunion and Toe Deformity?
A bunion, or hallux valgus as it is known in medical terms, is a condition that occurs when the big toe moves towards the lesser toes, creating a noticeable bony lump at the base of the toe. Consequently, this misalignment causes pain, swelling, difficulty putting on shoes, and indirectly leads to the formation of other defects like hammer toes or overlapping toes.
The occurrence of bunions may be attributed to hereditary predisposition, bad foot pattern, arthritis, or the continuous use of tight or narrow shoes. Besides, it should be noted that bunions are not solely cosmetic in nature; they are indicative of a structural defect that may progress to a more severe state over time.
What Is Minimally Invasive Bunion Surgery?
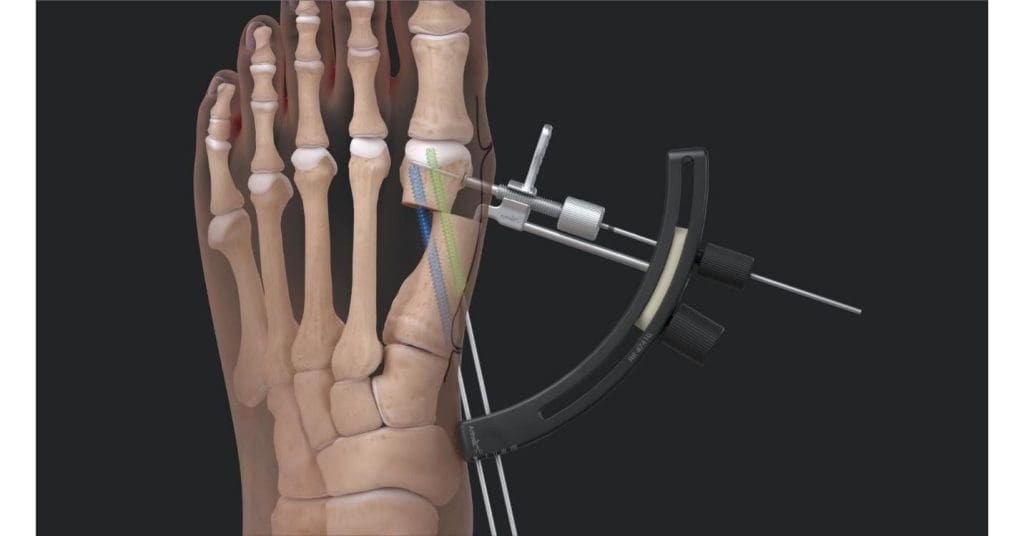
Minimally invasive bunion surgery (MIS) employs special instruments and tiny incisions, often only a few millimetres in length, to reposition the bones of the foot. MIS, in contrast to traditional open surgery, eliminates the need for large incisions and considerable dissection of the soft tissue.
Surgeons, through the use of real-time imaging guidance, can exactly rectify the deformity while still maintaining the integrity of the muscles, tendons, and blood vessels. This method significantly lessens the trauma caused to the foot while still achieving reliable alignment and long-term correction.
Minimally Invasive Techniques’ Key Benefits
Reduced post-operative pain is undoubtedly the most noticeable benefit of minimally invasive bunion surgery. The smaller incisions result in less tissue damage, which is a major factor contributing to the overall positive attitude of patients during the recovery period.
Patients enjoy:
- Less swelling and inflammation
- Scars that are hardly visible and look the same as good ones
- Quicker mobility and the ability to wear normal shoes sooner
- A decrease in the chances of wound complications
For a large number of people, all these advantages combined will lead to MIS becoming their first choice over traditional open surgeries, particularly if the procedure is done by a skilled bunion correction specialist.
Who Is a Suitable Candidate?
Bunion removal surgery performed through small incisions is not a one-size-fits-all procedure, and the selection for its use depends on various factors. The factors that determine the surgical decision are firstly, the degree of the deformity, and secondly, the condition of the joint, the presence of arthritis, and the overall alignment of the foot.
In general, bunions of a mild to moderate degree are recommended for MIS; however, with the recent advancements in technique, it is possible to correct in-place some severe deformities by minimally invasive methods as well. A very comprehensive clinical evaluation, along with imaging, is required to decide the best route for treatment.
What will happen on the day of surgery?
The micro-invasive procedure to remove bunions is usually done on an outpatient basis. The procedure can be done by either giving the whole body or just the foot anaesthesia, based on patient choice and the doctor’s judgment.
The surgeon changes the position of the bone through minute cuts and applies fixation to the changed position through internal means if necessary. Since the disruption of the soft tissue is very low, this procedure is usually shorter than conventional surgery.
Patients are generally allowed to put weight on the foot right after the operation, but in a protective post-operative shoe.
Recovery and Rehabilitation
Recovery time with open surgery is generally longer than minimally invasive intervention for bunion removal. In most cases, patients can put their weight on the operated foot immediately and, after a few days, can return to doing light daily chores.
The disappearance of swelling takes several weeks, and usually, after 4-6 weeks, patients are able to wear their normal shoes again. Physiotherapy could be suggested to regain the joint movement and to change the walking mechanics to a more efficient way.
Total recovery and bone healing take several months, but most patients feel a great improvement in the comfort and the foot shape very soon during the recovery process.
Long-Term Outcomes and Success Rates
When the surgeon is highly skilled, minimally invasive bunion surgery gives exceptional long-term results. Research indicates that using the right methods leads to high patient satisfaction, lasting correction, and low recurrence rates.
Simultaneous correction of the accompanying toe malformation further improves the outcome and eliminates the problem altogether. Regular foot care, wearing proper shoes, and following the post-operative instructions are the factors that together make the result last.
Choosing the Right Specialist Matters
The same as with any surgical procedure, the result is directly proportional to the surgeon’s skills. The surgeon must have specialised training and plenty of experience in the area to be able to do the difficult correction accurately and avoid complications.
Patients who are considering bunion surgery should consult with an orthopaedic surgeon who specialises in foot and ankle problems in particular, so that he can offer the right treatment according to the patient’s anatomy and lifestyle.

