Walk through a modern office, open a team chat, or sit in a late-night video meeting, and you can feel a strange contradiction. Work is more digital than ever, yet many people report being more mentally taxed than they were in roles that were physically harder. The language we use for this is often vague, like pressure, burnout, and overwhelm. But behind the emotion is a measurable biology story that public health increasingly treats as structural, not simply personal. That story is chronic stress and cortisol.
Cortisol is not a villain hormone. It is a core part of how the body helps you wake up, focus, mobilize energy, and respond to demands. Problems start when the workplace turns “short bursts of demand” into “continuous demand with no off switch.” That is where stress physiology can shift from helpful adaptation to wear and tear. The World Health Organization describes stress as a response to pressure and notes that chronic stress can worsen health and affect sleep, concentration, and behavior. The endocrine view is similar, too much stress without real danger can keep the body in a costly state.
The modern workplace did not create cortisol. It created a schedule and a culture that can keep cortisol relevant for too many hours of the day, too many days of the year.
Why cortisol became the symbol of work stress
Cortisol has become the headline because it sits at the center of the stress response. When the brain perceives a demand or threat, it triggers systems that increase alertness and energy availability, including cortisol. That makes cortisol easy to explain and easy to market.
But focusing only on cortisol levels can be misleading. Stress biology is more like a budget than a single number. Researchers often use the concept of allostatic load, the cumulative physiological burden from repeated or chronic stressors. Work-related psychosocial stress is one context where allostatic load has been studied, with attention to how chronic demands and low recovery time can translate into multi-system strain.
So the better question is not “Is my cortisol high?” The better question is, “Is my work design repeatedly activating stress pathways without enough recovery to return to baseline?” That is the heart of chronic stress and cortisol as a public health issue.
The workplace has changed in ways that make stress more chronic
Many jobs are less physically risky than before, yet several trends push stress toward chronicity.
Always in communication
Work no longer ends at the office door. Notifications follow people into evenings and weekends. Even when messages are not urgent, the possibility of urgency keeps attention partially engaged.
Ambiguous workload and invisible performance
In many roles, there is no clear finish line. Success is measured by responsiveness, speed, and the appearance of productivity. That ambiguity can feel like never being done.
High demand with low control
The job stress literature has long highlighted that high demands combined with low decision latitude can be toxic. NIOSH emphasizes that job stress is not just a personal weakness and discusses workplace conditions that can create stress, along with prevention strategies. (CDC)
Effort without predictable reward
People often tolerate high effort when rewards and recognition are consistent. When effort rises while reward feels unstable, the nervous system can treat work as a persistent uncertainty signal.
These conditions create a pattern where cortisol-related activation is not a short response to a clear threat. It becomes the background hum of daily life.
The health effects are broad because the stress response touches everything
When people talk about stress, they often reduce it to mood. Physiologically, long-term stress activation affects multiple systems. Mayo Clinic notes that long-term activation of the stress response system and too much exposure to cortisol and other stress hormones can disrupt many body processes and raise risk for problems, including sleep issues, weight gain, and cardiovascular issues.
This is why chronic stress and cortisol show up in so many different complaints at work.
A person may present with sleep disruption, then appetite changes, then more caffeine use, then reduced exercise, then escalating fatigue. None of those symptoms proves that cortisol is the cause. But stress-driven physiology can be a plausible thread linking them, especially when the work environment does not allow recovery.
A new angle on the crisis is measurement, not motivation
Workplace stress advice often sounds like personal improvement.
Meditate more
Do breathwork
Go for a walk
Drink less coffee
Those can help, but the public health angle asks a different question. Are we measuring the right things, and are we placing responsibility in the right place?
In research, chronic work stress is often studied through biomarkers and composite indices that capture multi-system burden, not only cortisol. The allostatic load approach has been used to understand physiological responses to work stress, including in recent studies of workers in high-stress contexts. Work stress and employee health reviews have also used the allostatic framework to organize evidence across pathways.
This matters because individual resilience can hide a problem until it does not. A worker can be high functioning for years while stress load accumulates. If organizations only track performance outputs and ignore recovery signals, they may discover the problem only when turnover rises, errors increase, and disability claims climb.
The cortisol rhythm problem occurs when the day never truly starts or ends
Cortisol follows a daily rhythm. In many people, it is higher in the morning and lower at night. Work patterns can disrupt the behaviors that support that rhythm, like consistent sleep timing and evening downshifts.
A simple example is the split-brain experiment.
A worker logs off at 7 pm but stays mentally active, checking updates, thinking about deadlines, and anticipating tomorrow’s meeting. That mental rehearsal can keep the body in readiness mode even when the person is physically at home. Over time, the gap between “I am off” and “My body is off” becomes the lived experience of chronic stress and cortisol.
This is why sleep is often the first casualty of work stress, and why sleep repair is often the first lever in recovery. WHO notes that stress can make it hard to concentrate and can contribute to trouble sleeping.
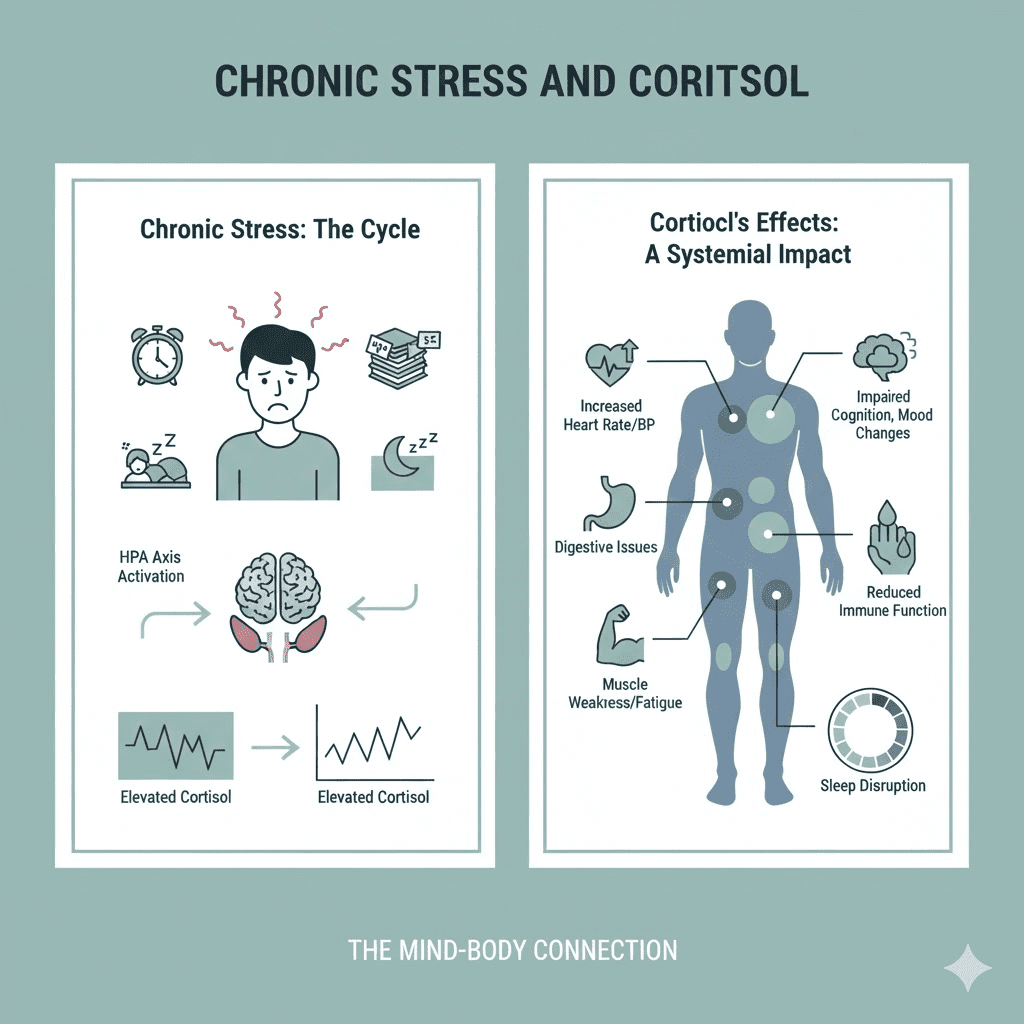
Why burnout is not just a mood state
Burnout is often treated as a personal failure, a lack of grit, or poor coping. A more accurate view is that burnout reflects a mismatch between demands and resources over time. Recent research continues to explore how chronic stress relates to burnout symptoms and why severity varies widely among employees.
The endocrine and public health significance is that burnout can be the visible tip of a chronic stress iceberg. Even if a person never reaches clinical burnout, sustained work stress can still influence health behaviors and physiological strain.
Where nutrition fits in a hormonal theme
A hormonal theme does not mean the answer is supplements. It means the body’s stress signaling is shaped by inputs, including nutrition, sleep, and activity.
In stress states, people often under-eat protein, skip meals, or rely heavily on ultra-processed snacks and stimulants. That pattern can amplify energy crashes and irritability, which then feed back into stress perception.
Nutrition is not a cure for a toxic workload. But nutrition can reduce the volatility that makes stress feel worse. In other words, food structure is not stress management, but it can be stress buffering.
This is one reason educators like Dr. Berg often bring up the connection between daily routines, metabolic stability, and how stressed people feel. If you want a practical starting point that connects routine building with health topics, you can read here.
What employers can do that is more effective than wellness slogans
NIOSH stresses that preventing job stress is not only about fixing workers, it is also about improving working conditions. That framing points to interventions that actually change stress exposure.
Clear boundaries on after-hours communication
This is not about banning messages. It is about defining what counts as urgent and building true overtime.
Workload visibility
When teams can see capacity and demand clearly, the brain treats work as more predictable and less threatening.
Control and autonomy where possible
Even small increases in decision latitude can reduce the feeling of helplessness that drives stress intensity.
Recovery baked into scheduling
Breaks, rotation, and meeting-free blocks are not perks. They are for physiological maintenance.
Management training in stress literacy
Leaders often escalate stress unintentionally through ambiguity, last-minute changes, and inconsistent priorities.
Public health has a clear interest here because the workplace is where adults spend a large share of waking life. When stress exposure is structural, structural fixes matter.
A grounded view of the crisis
The modern workplace stress story is not that people are weak. It is that work systems have evolved faster than human recovery systems.
The public health framing of chronic stress and cortisol is a call to stop treating stress as an individual hobby and start treating it as an exposure problem. WHO describes how chronic stress can affect health and behavior. NIOSH outlines workplace causes and prevention approaches for job stress. Clinical sources describe how prolonged stress hormone exposure can disrupt many body processes.
If you want a practical takeaway that respects the hormonal reality, it is this.
If recovery is not scheduled, it will not happen
If boundaries are not defined, the body stays on call
If stress is treated as a personal flaw, the exposure will continue
That is why the modern workplace has become a public health frontier. Not because cortisol is new, but because chronic activation has become normal.

